Authors / metadata
DOI: 10.36205/trocar7.2026007
Abstract
Background: Prolapsed cervical fibroids are rare and can mimic uterine inversion or even genital malignancy. When a large fibroid prolapses through the cervical canal or vagina, it may obscure the uterine fundus, complicating clinical diagnosis.
Case Presentation: The case of a 48-year-old woman with a large prolapsed cervical fibroid occupying the vagina, raising a suspicion of uterine inversion is presented. Diagnosis was confirmed intraoperatively. Surgical management included vaginal myomectomy followed by total abdominal hysterectomy due to distorted anatomy and persistent bleeding.
Conclusion: Prolapsed giant cervical fibroids are rare and may present with diagnostic confusion, particularly with uterine inversion. Accurate diagnosis and prompt surgical management are critical to prevent complications.
Introduction
Cervical fibroids represent less than 1% of all uterine fibroids. While submucosal and subserosal fibroids are more common, prolapse of a cervical fibroid into the vaginal canal is exceedingly rare (1). Large prolapsed fibroids can create diagnostic confusion, especially when accompanied by hemodynamic instability or traction on the uterus, mimicking acute or chronic uterine inversion or genital malignancy (2). Differentiating between these entities is crucial, as management varies significantly.
Case report
A 48-year-old parous woman presented to the emergency room of the Obstetrics and Gynecology Department of the tertiary care hospital with complaints of something coming out per vaginam for 20 days, progressively increasing in size, and increasing difficulty in walking and urination. She experienced the mass 20 days back after she tried to lift a heavy pot from the ground. She had a history of two vaginal deliveries, both uneventful. She gave a history of regular menses, every 30 days, lasting for 5-6 days with moderate flow, the last menses one month prior. She had no prior history of fibroid diagnosis or uterine surgery.
On Examination
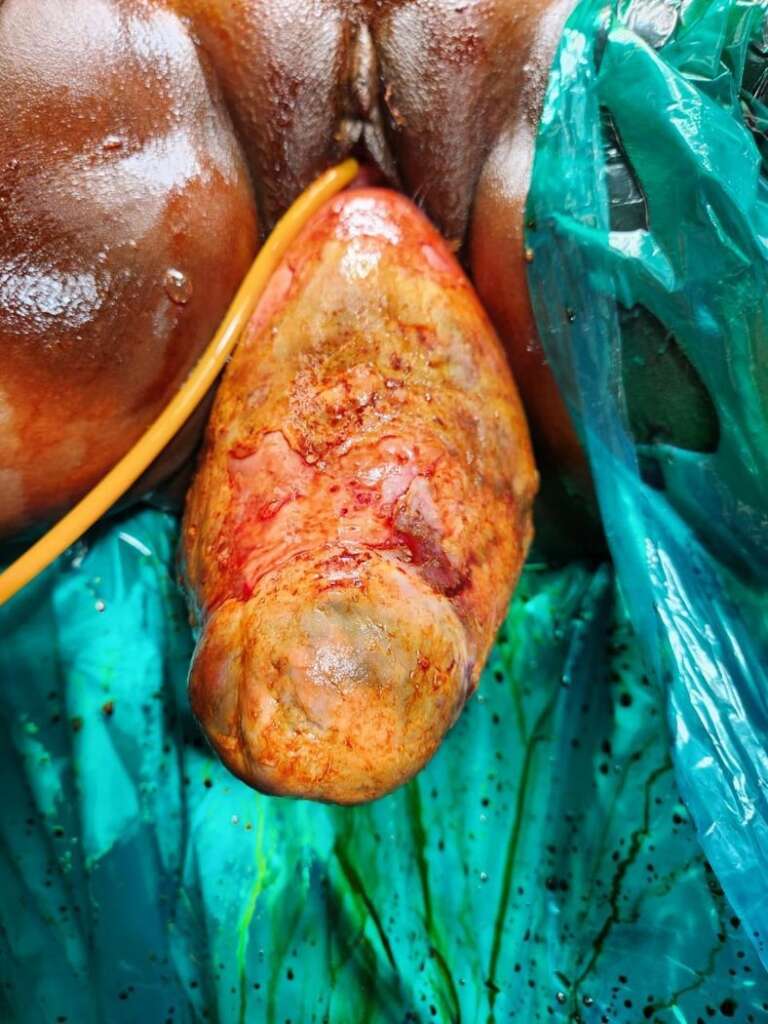
General condition: The patient was conscious, oriented to time, place, and person. Pulse-110/min, BP 118/70 mmHg, pallor present. Abdominal exam: soft, non-tender on palpation. Local exam: a large, necrotic, irregular, solid, infected foul-smelling mass (+/-20×15 cm) with degenerative changes was seen protruding from the introitus. The cervical os could not be identified (Fig 1). Bimanual exam was inconclusive: uterine fundus not palpable on abdominal or vaginal exam. The patient had been referred to a Cancer Specialty center in Mumbai to rule out malignancy, considering the exponential growth of the mass within three weeks. After ruling out malignancy on histopathology and immunohistochemistry, the patient was then referred to our tertiary care center for definitive management.
Investigations: Patient’s blood tests including tumor markers were within normal limits.
Pelvic Ultrasound: The cervix is bulky in size with a large 9.7 x 4.4 cm intraluminal lesion within it heterogenous in density. The uterus is normal in size and echotexture. Suggestive of a large cervical mass possibly neoplastic.
Pelvic MRI: Suggestive of a large pedunculated mass arising from the anterior lip of cervix with prolapse into the vaginal canal measuring approximately 5.4×9.7×15.9 cm – pedunculated cervical fibroid. The uterus is displaced posteriorly and is retroverted, the uterine body is unremarkable. No associated hematometra nor hydrometra is found. No obvious infiltration of the vaginal walls. No involvement of the urinary bladder, rectum, or sigmoid colon. There is no hydroureter. No suspicious locoregional lymphadenopathy or distinct metastatic disease is seen.
Histopathology (biopsy from the mass): Suggestive of spindle cell tumor of smooth muscle origin (leiomyomatous type) with focal atypia.
Immunohistochemistry from the mass: The tumor cells are diffusely positive for SMA, desmin and h-caldesmon while negative for S100 and SOX10. Tumor shows retained expression of ATRX protein. P53 shows wild type staining pattern. MIB1/Ki67highlights approximately 5-8% of tumor cell nuclei.
CT Thorax: Fibrobronchiectatic changes are seen in the inferior segment of the right middle lobe, No evidence of metastasis.
Management
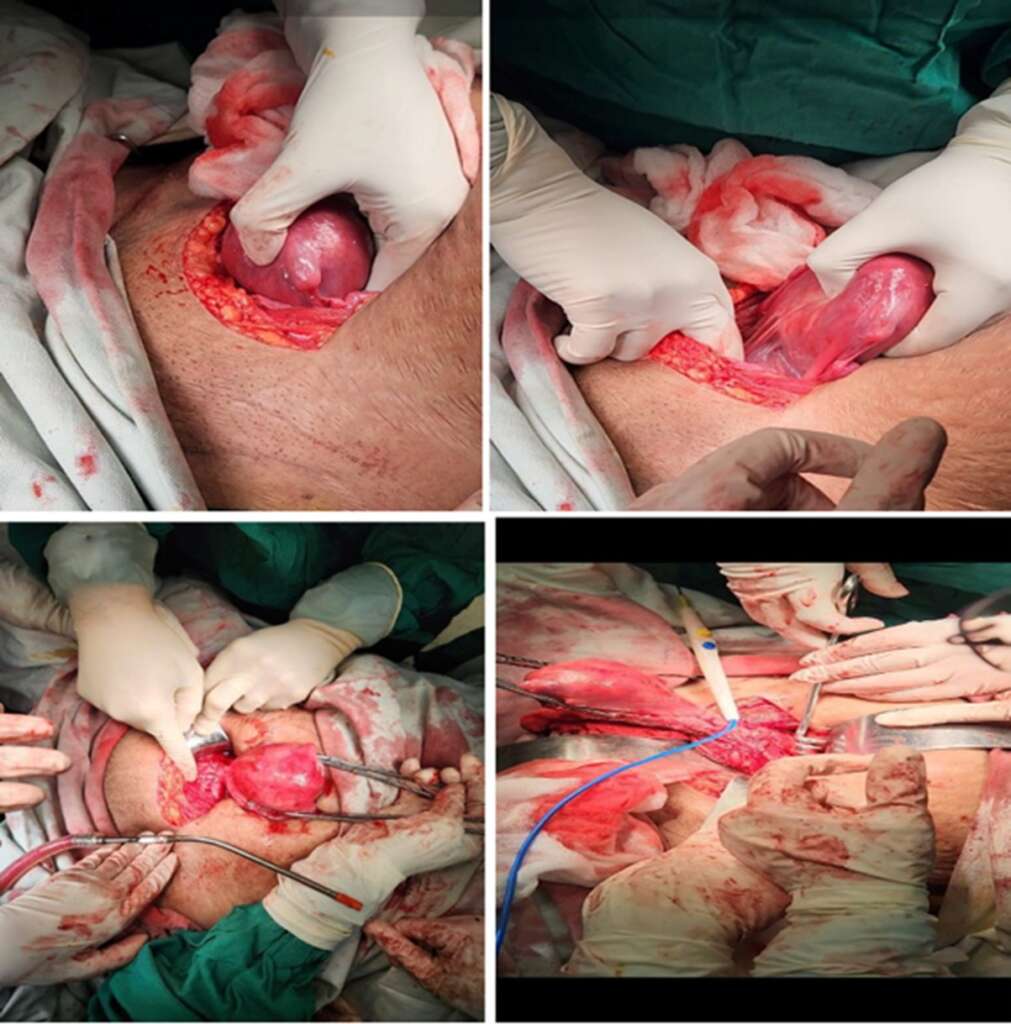
The patient was stabilized with broad-spectrum IV antibiotics, analgesics and with Betadine dressing of the protruding mass. The patient was planned for exploratory laparotomy with vaginal mass debulking with hysterectomy (abdominal/vaginal route). The patient and the relatives did receive an explanation regarding the risks and possible complications of the procedure. Examination under anesthesia (EUA) was done in lithotomy position covered by all aseptic precautions, the mass was confirmed to be arising from the anterior part of the cervical region. A laparotomy was performed to evaluate the pelvic anatomy, which revealed a large necrotic fibroid (+/- 20 x 15 cm) attached to the anterior cervical lip. No uterine inversion was noted. The uterus was enlarged and displaced inferiorly, the fallopian tubes were oedematous on both sides, the ovaries were normal bilaterally. Due to the weight of the cervical mass, proper visualization of the uterovesical fold was not possible, making the dissection extremely challenging. A debulking of the prolapsed cervical fibroid was done from the vaginal end, relieving the pressure from the uterus. A vaginal myomectomy was attempted but the mass was necrotic and bulky and hence could not be separated from the cervix. Therefore, the prolapsed mass was then pushed into the vagina and the uterine fundus was identified separately during abdominal exploration. An abdominal approach for hysterectomy was decided upon, which was performed including bilateral salpingectomy. Both ovaries were preserved. A peritoneal wash was performed. Bladder integrity was confirmed by the urologists through cystoscopy.
Histopathology: The cervix shows evidence of cervicitis. The Fallopian tubes are suggestive of acute salpingitis. The mass was diagnosed as a benign leiomyoma with areas of hyaline changes Occasional clusters of mature adipocytes are seen. The surface shows ulceration, fibrinosuppurative exudate and bacterial colonies. There was no evidence of atypia nor malignancy in the material examined.
Postoperative Course: Post operatively, the patient was kept on intravenous antibiotics and analgesics. Vaginal Betadine douching was done on day four and eight. On day ten, the patient had complaints of soaked abdominal wound dressing. On suture removal, the patient presented with a complete wound dehiscence up to the subcutaneous layer. The swab revealed staphylococcus aureus sensitive to amikacin and linezolid. Daily dressing was done under all aseptic precautions and high protein diet was advised. The patient was then taken for secondary resuturing of the wound under anesthesia on day seven of the wound dehiscence. She was then discharged on day three of post-resuturing the wound. On follow up, suture removal was performed on day 14 after resuturing. The patient appeared healthy and had no new complaints.
Discussion
Prolapsed cervical fibroids can present dramatically with bleeding, infection, and a mass per vaginam. Differentiating them from uterine inversion is difficult when the fundus is not palpable or when imaging is inconclusive. Inversion is typically associated with acute severe haemorrhage and shock, often postpartum, while cervical fibroid prolapse may have a subacute course (3). Imaging, especially MRI, helps to differentiate between the two. However, examination under anesthesia (EUA) and intraoperative findings remain the gold standard in many cases. In the patient presented, despite imaging and clinical confusion, a definitive diagnosis was made surgically. Anatomy of the ureters is expected to be distorted in cases of an impacted cervical fibroid. Hence meticulous dissection of the bladder coupled with careful application of clamps is a pivotal step in the surgery. In the case presented, the enucleation of the cervical myoma through the posterior incision on the uterocervical junction abdominally was the key surgical step in the surgery. This diagnostic confusion could have been prevented by presenting early at the hospital, where the patient could have been diagnosed and taken up for the myomectomy through the abdominal route without the risk of infection or necrosis of the mass. The surgical management of cervical myomas can be challenging and it requires a great experience, skill and expertise of the surgeon. The presence of a cervical leiomyoma has been identified as an independent factor affecting operation time in minimally invasive surgery (4). Identification of a correct cleavage plane for the surgeon becomes difficult in relation to the position of cervical myoma, as it can have close relations with pelvic structures, procedures can be further complicated by more restricted and inaccessible surgical spaces (5). Retrospectively, the assumption can be made that the post-operative wound dehiscence can be a consequence of the suppurative inflammation on the surface of the prolapsed myoma (as mentioned on the histopathology report) but the enucleation of the myoma was not possible vaginally due to the same reason hence the decision of abdominal hysterectomy had to be taken. Certain case reports with large cervical fibroid have been reported intermittently which eventually needed a hysterectomy after ruling out malignancy (6, 7, 8).
Conclusion
Prolapsed giant cervical fibroids are rare and may mimic uterine inversion, leading to diagnostic confusion. Careful examination, imaging, and surgical exploration are crucial. Early recognition and appropriate surgical planning can prevent morbidity and preserve patient’s safety. Their surgical management requires a multidisciplinary approach in modern era of surgery.